Handy tip: Vitamin D deficiency causes chronic inflammation (which means aging, dementia, bad stuff)
How many people have died of a vitamin D3 deficiency in the last 20 years?
If you are deficient in Vitamin D3, you may reduce chronic inflammation just by taking this five cent supplement and getting a bit of sun. A new study finds evidence that low levels of Vitamin D are not just linked, but cause the dreaded chronic inflammation which is so tied to aging that researchers talk about inflammaging in medical papers. The term captures the diabolic systemic effects of inflammation that accelerate aging, dementia and heart disease and a whole alphabet of other conditions. But don’t wait for your CDC, NHS, or AHPRA-approved-doctor to tell you. The global anti-inflammatory drugs market was worth USD 94 billion a few years ago. Imagine what it would do to that market if everyone sorted out their vitamin D levels?
Since Covid exacerbates inflammation, and people who are obese find it very hard to get their vitamin D blood levels up, it fits that aging, inflammation, obesity and low vitamin D3 make for a bad combination with SARS-2. And if inflammation causes some cases of Long Covid, then it seems to me that vitamin D3 may help with that too.
As I said in my big Vitamin D summary, Vitamin D influences over 200 genes. Vitamin D levels also correlate with lower rates of cancer, diabetes, high blood pressure, asthma, heart disease, dental caries, preeclampsia, autoimmune disease, depression, anxiety, and sleep disorders.
Combine it with Vitamin K2 as well to make sure the calcium ends up in your bones, not your arteries. (Though, people on blood thinners like warfarin need to get medical advice).
Down on Vitamin D? It could be the cause of chronic inflammation
The study examined the genetic data of 294 ,970 participants in the UK Biobank, using Mendelian randomization to show the association between vitamin D and C-reactive protein levels, an indicator of inflammation.
“This study examined vitamin D and C-reactive proteins and found a one-way relationship between low levels of vitamin D and high levels of C-reactive protein, expressed as inflammation.
“Boosting vitamin D in people with deficiencies may reduce chronic inflammation, helping them avoid a number of related diseases.”
Supported by the National Health and Medical Research Council and published in the International Journal of Epidemiology the study also raises the possibility that having adequate vitamin D concentrations may mitigate complications arising from obesity and reduce the risk or severity of chronic illnesses with an inflammatory component, such as CVDs, diabetes, and autoimmune diseases.
From the study itself (below) we get some idea of just how intricately tied D3 levels are to our immune system and all those inflammatory cytokines. To make life difficult, medical papers are always acronym-hell, and blood levels of vitamin D3 are referred to as “serum 25(OH)D”. And interleukins, which are the master messengers of the immune system are listed as IL-x. These molecules rapidly spread out and activate different white blood cells. There are 15 different interleukins in the human body, and at least 5 are affected by vitamin D.
Having sufficient Vitamin D might even neutralize some of the downsides of obesity or reduce the damage caused by CVD (cardiovascular disease), diabetes, allergies, etc. There’s no end to the sunshine good news, except that there is an obvious way to benefit millions of people, but our governments won’t do it.
Vitamin D is a pro-hormone. Its anti-inflammatory property captured by our analysis could be mediated through its hormonal effect on vitamin D receptor-expressing immune cells, such as monocytes, B cells, T cells and antigen-presenting cells.4 Indeed, cell experiments have shown that active vitamin D can inhibit the production of pro-inflammatory cytokines, including TNF-α, IL-1β, IL-6, IL-8 and IL-12, and promote the production of IL-10, an anti-inflammatory cytokine.4,5 Further, the anti-inflammatory effect also raises the possibility that having adequate vitamin D concentrations may mitigate complications arising from obesity and reduce the risk or severity of chronic illnesses with an inflammatory component, such as CVDs, diabetes, autoimmune diseases and neurodegenerative conditions, among others.1 If the related effects are indeed true, given the high prevalence of serum 25(OH)D levels of <50 nmol/L across the world (≤40% in some European countries),36,39–42 population-wide correction of low vitamin D status (e.g. by food fortification) could potentially be a cost-effective measure to reduce the burden of chronic disease. In fact, in linear MR analyses higher 25(OH)D concentrations have been associated with a lower risk of type 2 diabetes43 and multiple sclerosis (a chronic inflammatory disease of the central nervous system),44 with recent non-linear MR analyses providing evidence that correction of vitamin D deficiency can decrease the risk for CVDs15 and all-cause mortality.16
A recent study came out suggesting Vitamin D wasn’t any use to prevent broken bones, (see also Stop taking Vitamin D already!) but if researchers combine participants with high and low serum levels into one group, the results will be blurred to nothing — because people who are not deficient won’t benefit. I note neither story includes any mention of Vitamin K either (it almost looks designed to fail?).
In this experiment done at the University of SA, people were separated into high low and medium groups and the effect was clearly seen in the lowest group of <25nmol/L (which is a very low 10ng/ml level). [Convert your level here].
Having a severely low Vitamin D level sends the CRP levels through the roof
CRP or C-Reactive Protein is the standard marker of levels of inflammation. (Ask your doc, it’s a common blood test).
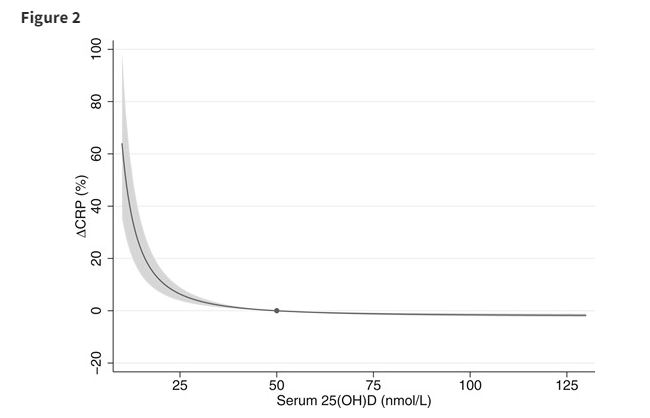
What makes the study a bit unusual is that it uses Mendelian randomization. It’s a technique to randomize things in medical experiments when it’s otherwise impossible or unethical to do a proper Randomized Controlled Trial (which is most of the time). It’s especially useful when we are trying to figure out which factor is the cause and which is effect, something that is notoriously difficult to do in the 30-variable-nightmare that is biology.
Mendelian Randomisation is a way to retrospectively randomize things — assuming that the genes were “randomly” assigned at birth and that the researchers don’t pick the wrong gene to study. (See the three assumptions listed under “Definition“.) Assuming the study was well done, it looks like a Vitamin D deficiency causes inflammation rather than inflammation causing a Vitamin D deficiency. It may not be the last word, but since Vitamin D is associated with a reduction in the holy grail of medical research — all-cause mortality — it’s probably better not to wait for the RCT which will never be done.
…
REFERENCE
Ang Zhou, Elina Hyppönen (2022) Vitamin D deficiency and C-reactive protein: a bidirectional Mendelian randomization study,
International Journal of Epidemiology, dyac087, https://doi.org/10.1093/ije/dyac087
9.2 out of 10 based on 50 ratings

Leave a comment